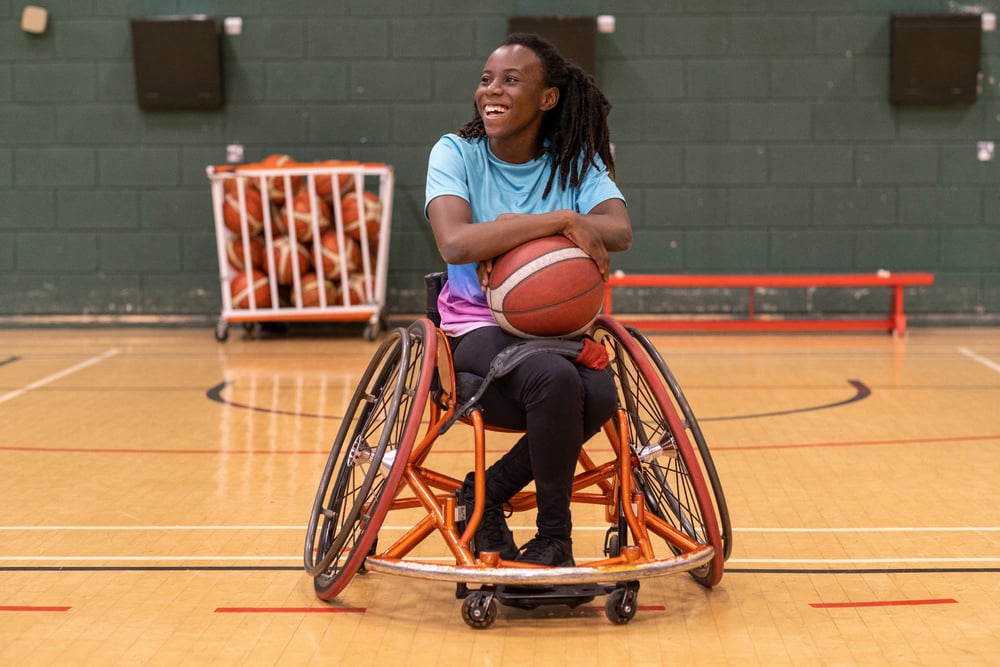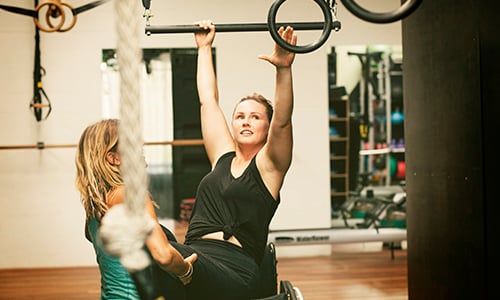Running out of medical supplies is one of the biggest concerns we hear from customers—and for good reason. Having what you need, when you need it, is essential to maintaining your health, independence, and peace of mind.
Reordering Medical Supplies Made Easy—and Stress-Free!
Apr 16, 2026 4:28:11 PM / by ABC Medical posted in independence, medical supplies, Work Life Balance, Health Tips, Living Well
Ostomy Support Belts: Do You Need One, and How Do They Help?
Mar 18, 2026 8:00:01 AM / by ABC Medical posted in independence, medical supplies, Health Tips, Living Well, Ostomy Care/Lifestyle
Living with an ostomy is a highly individualized experience. What feels essential to one person may not be necessary for another, especially when it comes to accessories like ostomy support belts. While not everyone with an ostomy needs a belt, many people find that the right support belt improves comfort, confidence, and overall quality of life.
Arthritis or Hand Weakness? Tools and Techniques to Make Catheterizing Easier
Mar 12, 2026 5:03:56 PM / by ABC Medical posted in independence, medical supplies, Health Tips, Living Well, Bladder Health
Living with arthritis, hand weakness, or limited mobility can make everyday routines more challenging. For people who use intermittent catheters, reduced grip strength or finger mobility can bring frustration and even discomfort into your daily catheterization routine.
Bathing & Swimming with an Ostomy: What’s Possible—and What’s Not
Mar 4, 2026 8:00:02 AM / by ABC Medical posted in Ostomy Care/Lifestyle
As a new ostomy user, you might wonder whether the activities that bring you joy, connection, and a sense of normalcy will still be possible. Adjusting takes time, but many new ostomy users discover that with the right preparation and support, the things they love are absolutely within reach.
On the Road Again: Driving with Spinal Cord Injury
Jan 20, 2026 3:38:08 PM / by ABC Medical posted in independence, spinal cord injury
There is no question driving has the ability to offer us a freedom unlike any other we enjoy. Whether traveling to pursue everyday activities or hitting the open road, driving is a privilege full of possibilities and, quite often, adventure.
Mobility Tips — Adaptive Driving
Jan 20, 2026 2:20:47 PM / by ABC Medical posted in independence, spinal cord injury
After your spinal cord injury, adaptive driving offers the opportunity to feel a little closer to some normalcy. Behind the wheel, there’s an obvious sense of freedom and independence. Those feelings of blending in and normality are invigorating for many drivers with paralysis.
6 Benefits of Exercise after a Spinal Cord Injury
Dec 29, 2025 1:33:52 PM / by ABC Medical posted in adaptive sports, motivation, active life, independent living, spinal cord injury, Health Tips
Once you’ve initially recovered from your spinal cord injury and have a daily routine, you may want to start an exercise program to keep you healthy and engaged while also managing your weight. Before embarking on any new activity, it’s always a good idea to have a clear idea of the benefits so that you can be motivated and energized.
12 Popular Wheelchair Sports & Activities
Dec 29, 2025 1:26:16 PM / by ABC Medical posted in adaptive resources, active life, adventure, independence, adapted sports, Health Tips, Living Well, mental health
It may surprise you to know that there are many different options for you to exercise and stay fit. Whether you want to compete in an individual or team sport as part of a league or local club, or if you’re looking for something to keep you physically active and manage your weight, there’s plenty to choose from.
Tennis, Anyone? Learn How to Ace Wheelchair Tennis
Dec 29, 2025 1:00:28 PM / by ABC Medical posted in wheelchair tennis, active life, independence, Health Tips, Living Well, mental health
Tennis is one of the fastest-growing wheelchair sports in the world. This court sport offers those with a spinal cord injury the opportunity to play in the same way and with the same rules as any tennis player, with one notable exception—the ball is allowed to bounce twice. This provides greater opportunities to make more shots, stay in longer rallies, and just have more fun!
Tips to Stay Active with a Spinal Cord Injury
Dec 29, 2025 12:45:33 PM / by ABC Medical posted in adaptive sports, motivation, active life, independent living, spinal cord injury, Health Tips
There are unique obstacles to exercise after a spinal cord injury, but it's vital to stay active. With a little motivation, staying fit can be easier and more fun than you may think.